When speaking with Mozziyar Etemadi, MD, PhD, one wouldn’t guess at his extensive academic background. He speaks without relying on jargon or overly technical terminology.
Yet his résumé is impressive: He has a master’s of science in electrical engineering from Stanford, a doctorate in bioengineering from UC San Francisco and UC Berkeley, and a medical degree from UC San Francisco. He’s now assistant professor of anesthesiology and engineering at Northwestern.
His background in a multitude of fields spanning engineering, medicine, and technology puts him in a unique position to take advantage of these powerful new tools. Also, he points out, his medical specialty, anesthesiology, is a discipline that collaborates with virtually every team in the hospital.
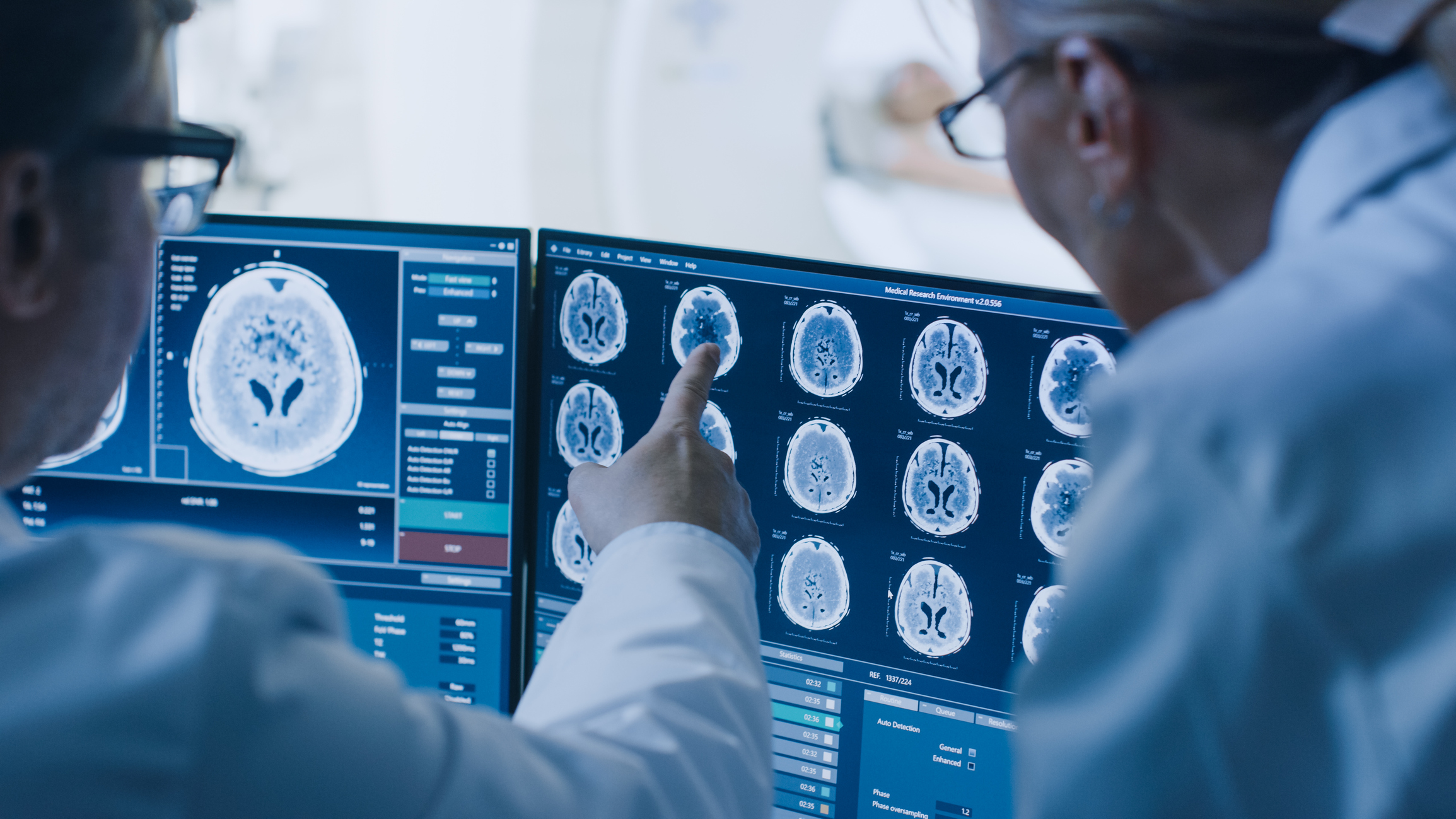
Etemadi and his colleagues fed their AI-based systems tens of thousands mammograms and CT scans until the computers were able to identify issues, on their own, in seconds.... with similar or better accuracy than the human eye.
“We work with surgeons, we work in the ICUs, we help deliver babies,” Etemadi says. “It’s a well-rounded foray, so when we’re developing these data tools, we have direct access to a lot of end users.”
So it perhaps wasn’t a surprise when the joint initiative he was working on for the last several years developed AI algorithms that use AI to read visual scans better than the human eye can. That system is now being tested in the real world, with the possibility of a wider roll-out in the near future.
Working with Google and the U.K. National Health Service, Etemadi and his Northwestern Medicine colleagues fed their AI-based systems tens of thousands mammograms and CT scans until the computers were able to identify issues, on their own, in seconds.
What’s more, the algorithms are able to identify problematic parts of an image with similar or better accuracy than the human eye.
The team celebrated this massive milestone success, but they didn’t dwell on it. Before long, they were drawing up plans for a clinical study to test their systems in the real world.
That trial is now running at Northwestern and will enable the algorithms to prove their merit not just retroactively when the outcomes are already known, but on a predictive basis as well.
The study will focus on breast cancer and will completely transform the current process for mammograms and follow-ups.
In the current system, patients have a mammogram done, then typically wait up to 30 days for it to be read by a specialist. If there are potential problems, the patient is contacted and they schedule a follow-up diagnostic mammogram, which “is a more intense mammogram essentially,” Etemadi says.
Then, depending on the availability of radiologists and hospital resources, the patient waits again until physicians can review the diagnostic scan and settle on a diagnosis.
But with the new algorithm, mammograms can be read by the computer within minutes. If a scan is flagged by the algorithm as high risk or problematic, the oncologist or radiologist can review it immediately and determine whether a diagnostic mammogram is necessary, before the patient has even gotten dressed.
With improved speed and efficiency, patients will experience less wait time and anxiety. Some research suggests that AI-based scan reading could help relieve some “scan-xiety” patients have when waiting for scan results.
The “re-ordering of the queue,” as Etemadi describes it, allows radiologists to spend more of their time on suspicious scans and drastically speeds up the process for patients when it comes to the identification of tumors or abnormalities.
The clinical study will also be key to understanding how the AI tools will be integrated and adopted by physicians, a task that’s just as critical as the effectiveness of the tools themselves.
“It’s really important to take time and make sure that the interaction between the human and the tool is as good as it possibly can be,” Etemadi says.
With improved speed and efficiency, patients will experience less wait time and anxiety. Some research suggests that AI-based scan reading could help relieve some “scan-xiety” patients have when waiting for scan results.
With a smart tool like AI, radiologists will be able to focus more on critical scans, and their workload will be handled more efficiently.
That’s especially important given how high in demand cancer screening is today. And ultimately, patient outcomes may improve — more tumors will be caught, and they’ll be caught earlier.






-min.jpg)








